National Breast Cancer Awareness Month: Breast Cancer Malpractice Concerns
Kristy Kramp, J.D., LHRM // October 22, 2017
Since 1985, October has been internationally recognized as Breast Cancer Awareness Month. Throughout the month, pink ribbons are prominently displayed on thousands of products, from apparel to office supplies, and millions of individuals participate in fundraising events to raise awareness and funds for the cause. Awareness is more than just wearing pink. For physicians, its knowledge of not only the clinical side of the disease but also the rising associated malpractice risks for diagnosis and treatment.
Breast Cancer Facts
- 1 in 8 women in the U.S. will be diagnosed with breast cancer in her lifetime.
- Breast cancer is the most commonly diagnosed cancer in women.
- Breast cancer is the second leading cause of cancer death among women.
Breast Cancer Malpractice Claims
Ninety-two percent of breast cancer malpractice claims are caused by a failure to diagnose or a delay in diagnosis. The specialties that are primarily at risk for claims are radiology, family practice/internal medicine, gynecology, general surgery, and pathology.
The top contributing factors in missed or delayed diagnosis of breast cancer are patient assessment issues and patient factors. Patient assessment issues include misinterpretation of diagnostic studies, failure or delay in ordering diagnostics, inadequate patient assessment to rule out abnormal findings, failure to respond to continued symptoms and patient concerns, inadequate history and physical, and overreliance on negative diagnostics, despite the presence of clinical findings.
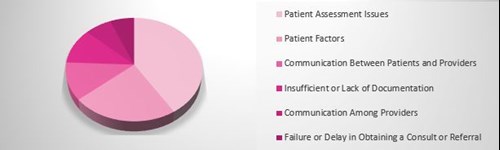
Greenberg P, Ranum D, Siegal D. Navigating Risk in Breast Cancer Diagnosis and Treatment. PSQH. Oct 12, 2015
Risk Management for Breast Care
Self-detected mass: Most failure to diagnose breast cancer cases involve a patient-detected mass, lump, or thickening. A patient-detected lump should be followed to conclusion, even if its presence cannot be confirmed.
Negative Finding: Engage patient in a discussion about breast care management following negative test/imaging results. Develop a clear and effective plan, and ensure patient’s understanding and agreement of that plan.
Risk Factors: Assessment, and periodic updating, of a patient’s personal and family history ensures timely breast cancer screening, including appropriate referrals to high risk counseling.
Test Results: Primary care providers and radiologists must coordinate the process for communication of all test results to the patient and for confirming receipt of all results by the ordering provider.
Follow up: Document recommendations for follow-up testing and communicate the follow-up plan to the patient and all responsible providers.
Documentation: Thoroughly document breast examinations and include, in quotes, the patient’s breast-related complaints. Diagram the exact location of all confirmed lumps or lesions. For unconfirmed masses, record the location and nature of the complaint, using the patient’s own words.
Referrals: For patients referred to a specialist, ensure coordination of care among all providers and clearly explain the roles and responsibilities to the patient.